📝Comment:
This meta-analysis represents the highest level of evidence for a prognostic biomarker, using Individual-Participant-Data (IPD) analysis across 15 high-quality prospective cohorts.
While the absolute increase in risk prediction (C-index) is modest, high-sensitivity troponins are an independent prognostic factor for cardiovascular disease that provide greater predictive gains than traditional inflammatory markers like C-reactive protein (CRP), and kidney function (eGFR).
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line:
This large-scale individual-participant-data (IPD) meta-analysis demonstrates that high-sensitivity cardiac troponins (cTnT and cTnI) are independent prognostic markers for cardiovascular disease (CVD) in the general population. While adding troponins to conventional risk factors (age, sex, smoking, lipids, blood pressure) yields a statistically significant improvement in risk prediction, the absolute magnitude of this improvement is modest (C-index increase of ~0.012 to 0.015).
Modeling suggests a potential population health benefit: restricting troponin screening to individuals at “intermediate risk” could prevent 1 additional CVD event for roughly every 400–470 people screened, provided this reclassification triggers statin therapy. Clinically, troponins perform better than C-reactive protein (CRP) and kidney function (eGFR) for risk discrimination, but offer similar predictive value to NT-proBNP.
Results
Summary of Results:
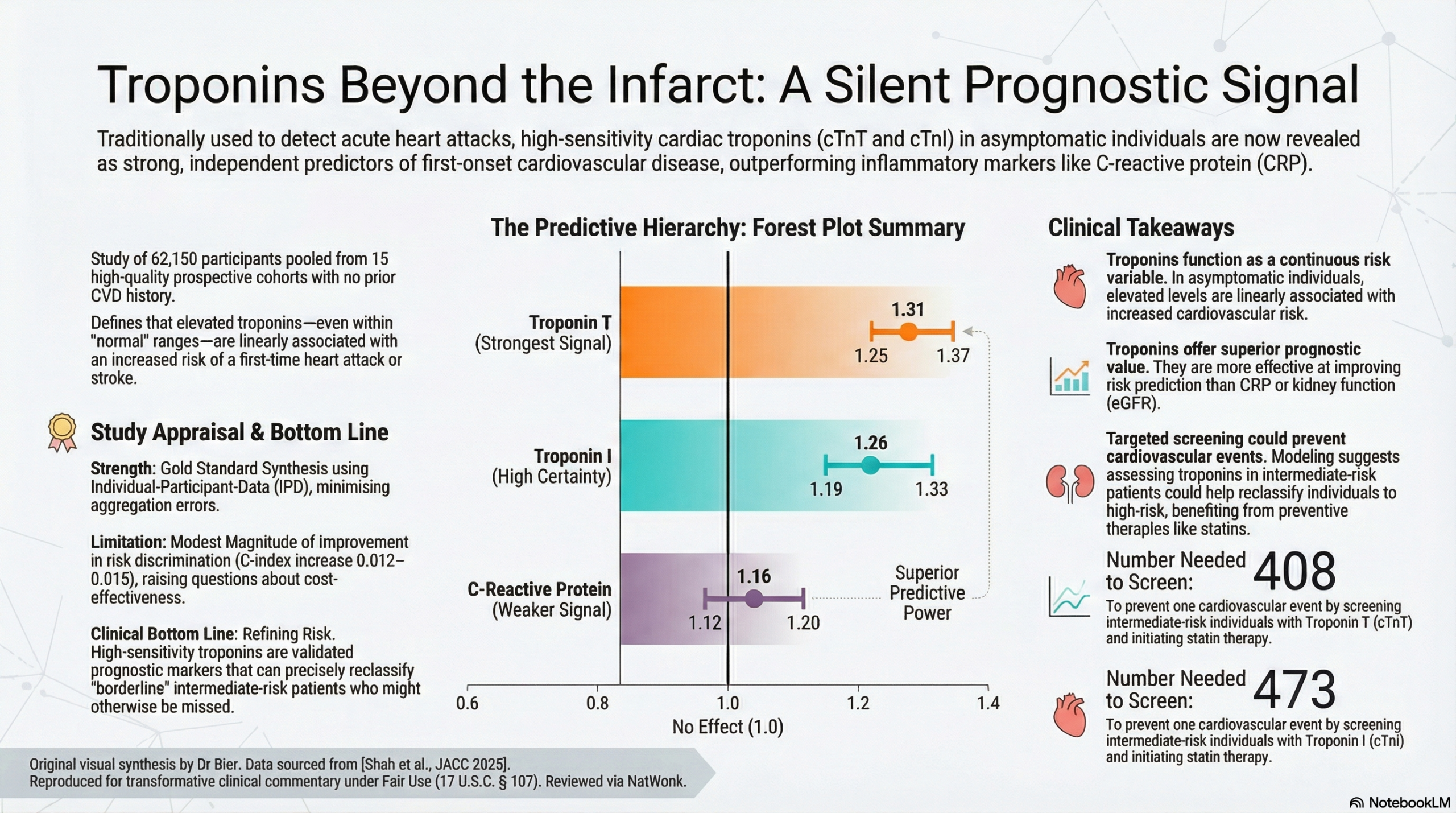
- Association with CVD: In a pooled analysis of 62,150 participants without prior CVD, higher baseline troponin concentrations were linearly associated with increased CVD risk.
- Hazard Ratio (cTnT): 1.31 (95% CI: 1.25–1.37) per 1-SD higher concentration.
- Hazard Ratio (cTnI): 1.26 (95% CI: 1.19–1.33) per 1-SD higher concentration.
- Incremental Risk Discrimination: Adding troponins to standard risk factors improved the C-index (a measure of how well the model separates cases from non-cases).
- cTnT addition: +0.015 (95% CI: 0.012–0.018).
- cTnI addition: +0.012 (95% CI: 0.009–0.015).
- Population Health Modeling (UK Context): Using data from 2.1 million UK primary care patients, the authors estimated the impact of a “targeted” strategy (screening only those at intermediate 10-year risk).
- Number Needed to Screen (NNS): To prevent one CVD event over 10 years (assuming statin initiation), the NNS was 408 for cTnT and 473 for cTnI.
- Biomarker Comparison: Troponins provided greater predictive gains than CRP or eGFR, but were broadly comparable to NT-proBNP10. Adding troponin to NT-proBNP did not yield additive value, suggesting overlapping pathophysiological signals.
Assertive Critical Appraisal
Certainty of Evidence (GRADE Framework Adaptation):
The certainty of the prognostic association is High. This is an Individual-Participant-Data (IPD) meta-analysis—the “gold standard” of evidence synthesis—allowing for consistent harmonization of variables across 15 high-quality prospective cohorts.
Magnitude of Effect vs. Statistical Significance:
While the C-index improvements are statistically significant (p < 0.001), they are numerically small (around 0.01). In risk prediction literature, improvements of this magnitude are often considered marginal for changing clinical practice across a whole population. However, the authors effectively use reclassification analysis (NRI) to demonstrate that this small statistical gain could still translate into meaningful reclassification of intermediate-risk patients into high-risk categories where treatment is indicated.
Prognostic vs. Predictive Utility:
It is critical to distinguish the claims here.
- Prognostic (Established): The study definitively proves troponins are prognostic (they predict who will have an event).
- Predictive (Modeled): The claim that screening prevents events is based on a simulation assuming that identifying high risk leads to statin use, and that statins reduce risk by 20%. This is not a randomized trial testing troponin-guided therapy against standard care.
Heterogeneity and Assay Standardization:
The study combined data using different high-sensitivity assays (Roche for cTnT, Abbott for cTnI). While they found similar predictive ability for both, the inability to perform head-to-head comparisons in most cohorts (only two cohorts measured both) is a limitation.
Applicability and Generalizability:
The cohorts were predominantly of European ancestry (Europe and North America). The risk modeling was calibrated specifically to the UK primary care population. Therefore, the specific “Number Needed to Screen” estimates may not directly apply to diverse populations with different baseline CVD risks or healthcare systems. Furthermore, the analysis did not compare troponins against newer algorithmic standards like QRISK3 or PREVENT, which may already capture some of this risk through other variables.
Reporting Quality Assessment (TRIPOD/PRISMA):
The study adheres to TRIPOD guidelines for prediction models. The authors utilized robust methods to handle limit-of-detection values and non-linear associations, enhancing the validity of the statistical conclusions.
Research Objective:
To quantify the incremental value of adding cardiac troponins (cTnT and cTnI) to conventional cardiovascular risk factors for the prediction of first-onset CVD and to model the potential population health impact of such screening.
Study Design:
- Design: Individual-Participant-Data (IPD) Meta-Analysis of prospective cohort studies.
- Modeling Component: Simulation of screening impact using electronic health records from the UK Clinical Practice Research Datalink (CPRD).
Setting and Participants:
- Cohorts: 15 prospective cohorts from Europe (65%) and North America (33%).
- Sample: 62,150 participants with no history of CVD at baseline.
- Follow-up: Median follow-up was 11.8 years for cTnT cohorts and 9.8 years for cTnI cohorts.
Bibliographic Data:
Author: Shah ASV, Keene SJ, Pennells L, et al.
Title: Cardiac Troponins and Cardiovascular Disease Risk Prediction.
Journal: Journal of the American College of Cardiology.
Year: 2025; 85(14): 1471-1484.
DOI: 10.1016/j.jacc.2025.02.016.
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
