Comment:
Although we are all used to seeing troponin used to rule in or out a heart attack, this study shows it can be used for prognostic chronic risk stratification. It shows there is a population of older, asymptomatic people who, despite having no history of MI or overt CVD, are walking around with a cardiac risk profile equivalent to someone already diagnosed with heart disease. It’s essentially an early warning system that shows the heart is under constant, chronic stress.
Summary:
Clinical Bottom Line
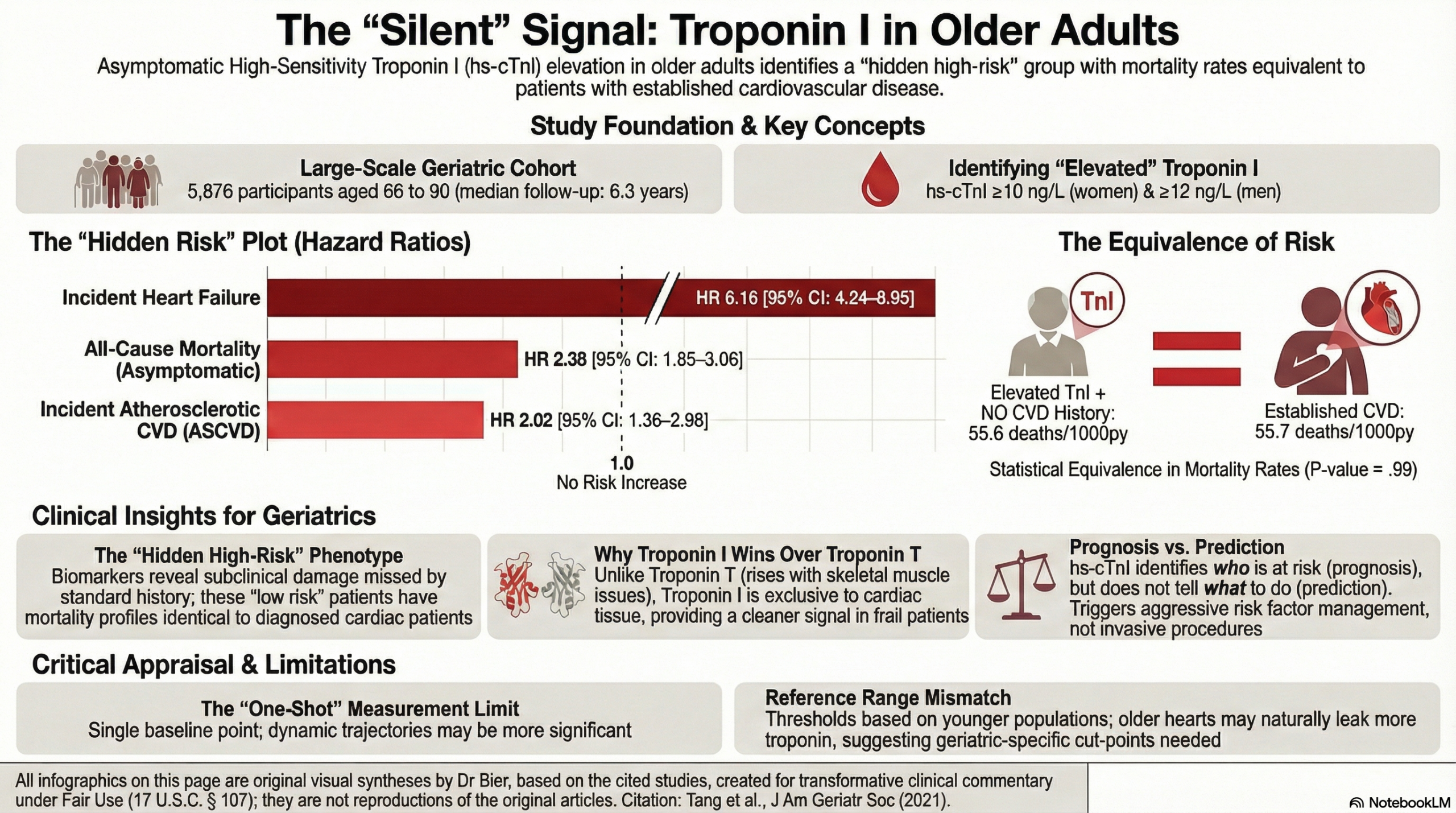
This prospective cohort study from the ARIC investigators provides robust evidence that high-sensitivity cardiac troponin I (hs-cTnI) is a potent prognostic marker in older adults (ages 66–90). Its most clinically striking finding is that asymptomatic older adults with elevated hs-cTnI—but no history of cardiovascular disease (CVD)—face a mortality risk statistically equivalent to patients with established CVD.
While hs-cTnI improves risk stratification beyond traditional factors (like cholesterol and blood pressure), clinicians must recognize that this study establishes prognosis (risk prediction), not prediction of treatment response. Elevated hs-cTnI identifies a vulnerable “hidden high-risk” geriatric population, particularly for future heart failure, but the study does not define a specific therapeutic algorithm for these patients beyond general intensive risk factor management.
Results in Context
Main Results
The study followed 5,876 older adults for a median of 6.3 years3. The associations between hs-cTnI levels and adverse outcomes were substantial, particularly for those without baseline CVD:
-
All-Cause Mortality: Participants with elevated hs-cTnI (but no prior CVD) had a more than two-fold increase in mortality risk compared to those with low levels (Adjusted Hazard Ratio [HR] = 2.38; 95% CI: 1.85–3.06).
-
Incident Heart Failure: This was the strongest association observed. Elevated hs-cTnI was associated with a 6-fold increase in the risk of developing heart failure (HR = 6.16; 95% CI: 4.24–8.95).
-
Incident Atherosclerotic CVD (ASCVD): Elevated levels were associated with a doubled risk of ASCVD (HR = 2.02; 95% CI: 1.36–2.98).
Biomarker Comparison (hs-cTnI vs. hs-cTnT)
The study compared Troponin I (TnI) to Troponin T (TnT). Hs-cTnI showed greater improvement in model discrimination (C-statistics) for incident heart failure and global CVD compared to hs-cTnT.
Definitions & Context
-
Prognostic vs. Predictive: This study validates hs-cTnI as a prognostic marker (it predicts the natural history of the patient). It was not tested as a predictive marker (which would indicate who responds better to a specific drug, such as a statin).
-
High-Sensitivity Assay: Unlike standard troponin tests used to diagnose heart attacks, high-sensitivity assays can detect very low levels of troponin released due to subclinical chronic damage (e.g., cell turnover, apoptosis) rather than acute ischemia.
Assertive Critical Appraisal
Appraisal of Biomarker Claim (Prognostic vs. Predictive)
The authors appropriately frame hs-cTnI as a tool for risk stratification (prognostic) rather than guiding specific therapy.
-
Strength: The comparison with hs-cTnT is a critical methodological strength. The authors rightly note that hs-cTnT can be elevated in skeletal muscle regeneration and myopathies. By showing that hs-cTnI (which is exclusive to the heart) performs better for heart failure prediction, the study offers a more specific tool for cardiac risk in older adults who may have comorbid frailty or sarcopenia.
-
Limitation: The study relies on a single baseline measurement. It does not account for the “delta” or trajectory of troponin over time, which recent literature suggests may be even more prognostic than a static value.
Reporting Quality Assessment (REMARK)
The reporting generally aligns with REMARK guidelines, but specific caveats apply:
-
Assay Cut-points: The study used manufacturer-defined sex-specific reference ranges (Women: ≥10 ng/L; Men: ≥12 ng/L for “elevated”). While practical, these cut-points were derived from healthy reference populations and may not be optimized specifically for an older (66-90 year old) cohort where baseline troponin leak is naturally higher.
-
Confounding Control: The statistical models were rigorous, adjusting for key confounders including eGFR (using Cystatin C, which is more accurate in the elderly) and NT-proBNP. This strengthens the conclusion that troponin provides signal independent of kidney function or wall stress.
Applicability
The findings are highly applicable to general practice as hs-cTnI assays are FDA-approved and widely available. However, the clinical “next step” remains ambiguous. While the authors suggest “more intensive cardiovascular risk management”, clinicians should be careful not to over-interpret an elevated hs-cTnI as a mandate for invasive testing (like catheterization) in asymptomatic patients, given the lack of evidence for such a strategy in this specific context.
Research Objective
To assess whether high-sensitivity cardiac troponin I (hs-cTnI) independently predicts mortality and cardiovascular risk in older adults beyond traditional risk factors, and to compare its performance against high-sensitivity cardiac troponin T (hs-cTnT).
Study Design
-
Design: Prospective cohort study (Analysis of Visit 5 data from the ARIC study).
-
Comparison: Participants stratified by sex-specific hs-cTnI categories (Low, Moderate, Elevated).
-
Endpoints: All-cause mortality, cardiovascular mortality, incident global CVD, incident ASCVD, and incident heart failure.
Setting and Participants
-
Setting: Community-based population from four U.S. communities (ARIC Study).
-
Participants: 5,876 older adults, aged 66 to 90 years.
-
Demographics: 42% male, 23% Black, 24% with prevalent CVD.
Bibliographic Data
-
Title: High-Sensitivity Cardiac Troponin I for Risk Stratification in Older Adults
-
Authors: Tang O, Matsushita K, Coresh J, Hoogeveen RC, Windham BG, Ballantyne CM, Selvin E.
-
Journal: J Am Geriatr Soc.
-
Year: 2021 (Author Manuscript version provided)
-
DOI: 10.1111/jgs.16912
Original Article:
Full text: PubMed Central
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
