Comment:
This is a powerful meta-analysis that validates what we and our patients have known for decades. The data is clear: patients overwhelmingly prefer combination therapy, and the network meta-analysis highlights that desiccated thyroid extract (DTE) is the most preferred intervention of all.
What’s particularly telling is the discrepancy between patient preference and the results from standardized quality-of-life questionnaires. This doesn’t invalidate the patient’s preference; it invalidates the questionnaires. Our measurement tools are clearly not sensitive enough to capture the full spectrum of symptomatic relief that patients experience when their T3 levels are properly restored.
This paper serves as yet another significant piece of evidence against the “one-size-fits-all” T4 monotherapy approach. It provides a robust, data-driven argument for listening to our patients and offering DTE as a primary, legitimate, and—as the evidence suggests—often superior, therapeutic option.
Summary:
Clinical Bottom Line
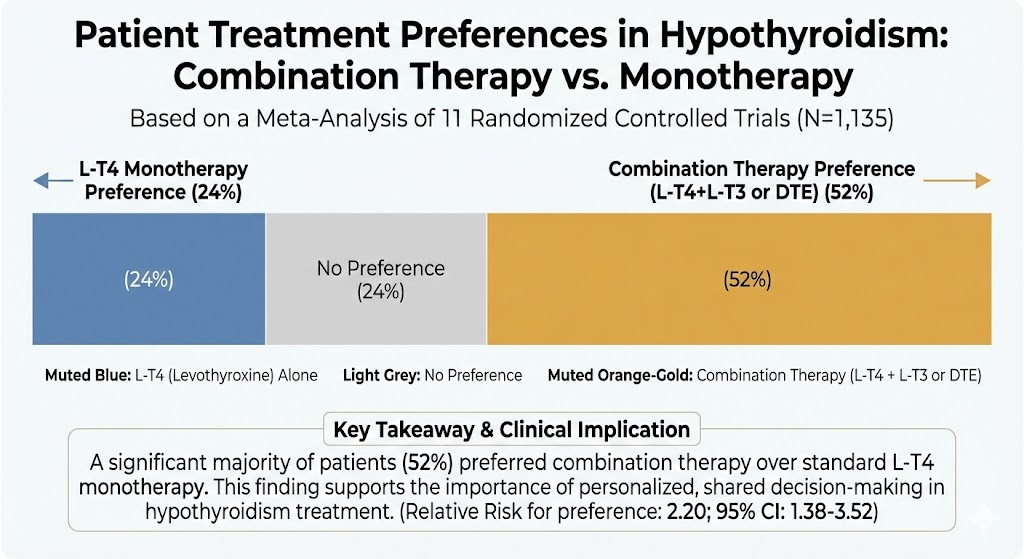
This meta-analysis of 11 randomized controlled trials (RCTs) found that patients with hypothyroidism significantly prefer combination therapy (either L-T4 + L-T3 or desiccated thyroid extract [DTE]) over standard L-T4 monotherapy. Overall, 52% of patients preferred combination therapy, while only 24% preferred monotherapy and 24% had no preference. This finding is notable because many of the individual trials included in the analysis failed to show any significant difference in quality-of-life questionnaires or other patient-reported outcomes (PROs), suggesting a discrepancy between standardized questionnaires and overall patient preference. The authors conclude that this strong preference justifies considering combination therapy as part of a shared decision-making process.
Results
-
Summary of Results: The primary meta-analysis of all 11 RCTs (1135 patients) found that patients were more than twice as likely to prefer combination therapy over L-T4 monotherapy (Relative Risk [RR]: 2.20; 95% CI, 1.38-3.52).
-
Network Meta-Analysis (NMA): A network meta-analysis (NMA) was used to compare all three treatment types (L-T4, L-T4 + L-T3, and DTE) simultaneously. This analysis also found that both L-T3 + L-T4 (RR: 1.90) and DTE (RR: 2.34) were significantly preferred over L-T4 monotherapy. Across all studies, DTE had the highest probability (84%) of being the most preferred intervention.
Assertive Critical Appraisal
-
Certainty of Evidence (GRADE Framework): The authors do not use the formal GRADE system; however, based on their own analysis, the certainty of this evidence should be considered Moderate. The main reason for downgrading is the substantial heterogeneity (I² = 81%) observed in the initial analysis, indicating significant differences in the results of the included studies.
-
Heterogeneity: The initial analysis showed substantial heterogeneity (I² = 81%). I² represents the percentage of variation across studies that is due to real differences in effect rather than just chance. The authors appropriately addressed this by conducting a sensitivity analysis: they removed 4 studies identified as primary sources of heterogeneity. This reduced the I² markedly to 24% and, importantly, the result remained statistically significant and robust (RR: 1.97; 95% CI, 1.52-2.54), which strengthens confidence in the primary finding.
-
Publication Bias: The authors assessed for publication bias using Egger’s test and visual inspection of funnel plots. They reported finding no evidence of publication bias, which increases confidence that the pooled estimate is not overly inflated by missing negative studies.
-
Risk of Bias in Included Studies: The authors used the Cochrane Risk of Bias tool (RoB V.2.0). Of the 11 included RCTs, 4 were judged as having a low risk of bias, 6 had “some concerns,” and 1 had a high risk of bias. This mixed quality is a common finding in meta-analyses but suggests the pooled evidence is not derived exclusively from high-quality trials.
-
Special Consideration (Pooled vs. Individual Results): It is important to note that while the overall pooled result is statistically significant, the authors report that the majority of the individual studies (6 of 11) did not find a statistically significant difference in preference on their own. This scenario often occurs when individual studies are underpowered (i.e., too small) to detect a modest but real treatment effect. By combining their data, the meta-analysis increases the overall statistical power, which can reveal a consistent trend that was not apparent in the smaller studies. However, this finding must be interpreted with caution, especially given the high initial heterogeneity, which suggests real differences between the trials.
-
Reporting Quality Assessment (PRISMA): The review adheres to PRISMA reporting guidelines. It includes a complete PRISMA flow diagram (Fig. 1) detailing the study selection process and provides a description of the database search strategy. This enhances the transparency and reproducibility of the review.
Research Objective
The study’s objective was to assess patient preferences in the treatment of hypothyroidism, using the following PICO framework:
-
Population: Adult patients (age ≥ 18) with overt primary hypothyroidism.
-
Intervention: Combination therapy (synthetic L-T4 + L-T3 or DTE).
-
Comparator: L-T4 monotherapy.
-
Outcome: Patient preference for treatment.
Study Design
The authors conducted a systematic review, meta-analysis, meta-regression, and network meta-analysis of randomized controlled trials. They searched the PubMed, Embase, and Cochrane databases for studies published up to April 10, 2024. The review included parallel or crossover RCTs that compared combination therapy to L-T4 monotherapy and explicitly evaluated patient preference as an outcome.
Setting and Participants
The analysis included a total of 11 RCTs, 8 of which were crossover studies. These trials enrolled a combined total of 1135 patients.
Bibliographic Data
-
Title: Treatment Preferences in Patients With Hypothyroidism
-
Authors: Fabyan Esberard de Lima Beltrão, Giulia Carvalhal, Daniele Carvalhal de Almeida Beltrão, Fabricia Elizabeth de Lima Beltrão, Miriam O. Ribeiro, Matthew D. Ettleson, Helton Estrela Ramos, and Antonio C. Bianco
-
Journal: The Journal of Clinical Endocrinology & Metabolism
-
Year: 2025 (Advance access publication: 18 September 2024)
This AI-generated analysis is for informational and research purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified health provider with any quest1ions you may have regarding a medical condition.
Original Article:
Full text: here
