Comment:
I always prioritize all-cause mortality data over mechanism, and the hypothesis that sun exposure is negative is at this point dogmatic. This 2018 review is another showing the prevailing clinical mandate for UV avoidance conflicts with the documented reality that sun avoidance is a negative factor for human longevity.
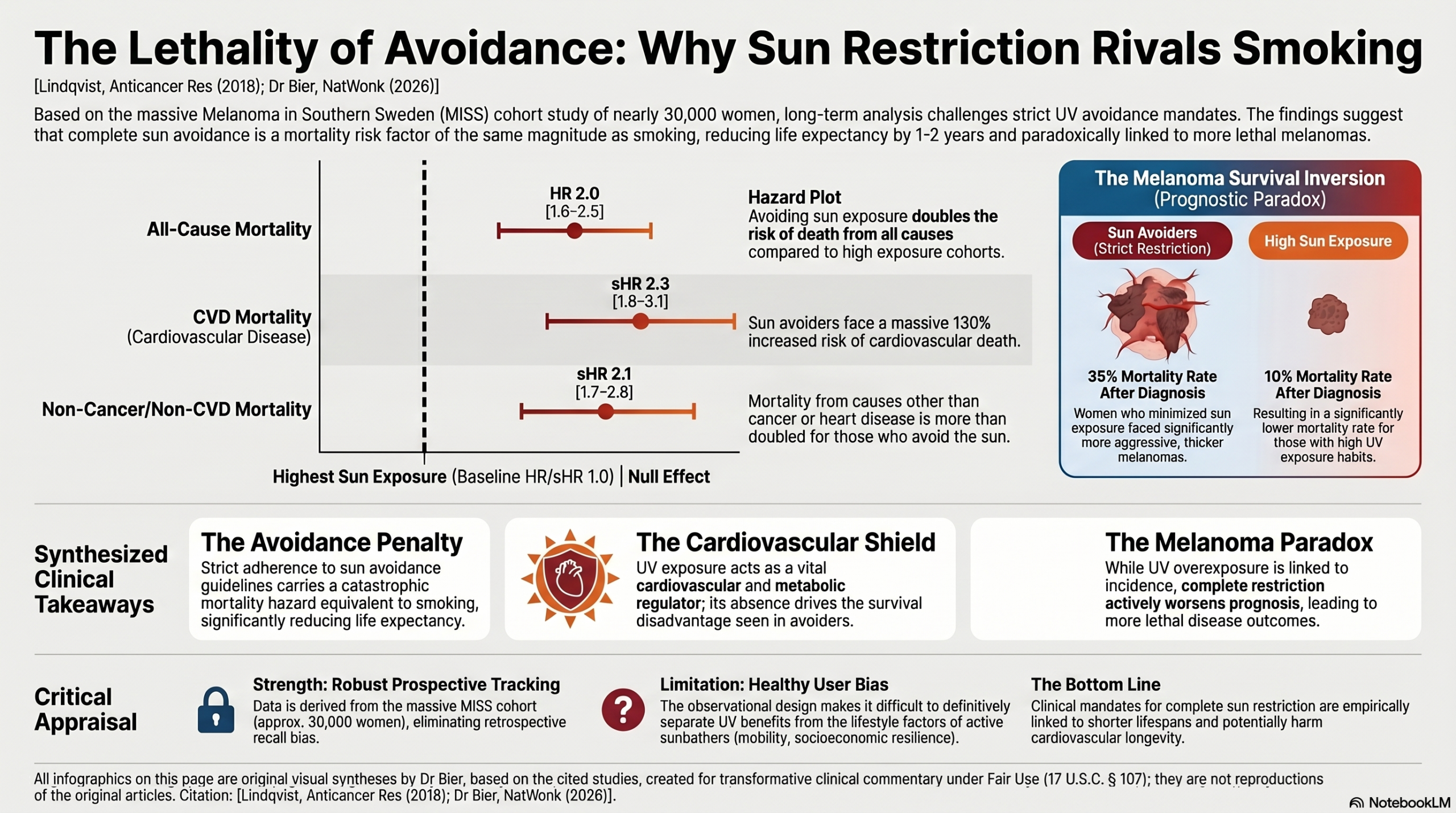
The Melanoma in Southern Sweden (MISS) cohort data reveals a stark structural reality: women who avoided sun exposure faced a two-fold increase in mortality rate compared to those in the highest exposure group (HR = 2.0; 95% CI: 1.6–2.5). Most provocatively, the data suggests that sun avoidance is a risk factor for death of a similar magnitude to smoking. In a clinical landscape where we spend billions to mitigate smoking-related harm, we should question why we are actively prescribing a behavior (UV avoidance) that yields a similar mortality hazard.
While episodic UV overexposure is linked to melanoma incidence, the review confirms a critical prognostic inversion: low sun exposure and deficient vitamin D levels are associated with thicker, more aggressive melanomas. The mortality gap is staggering—35% of women with low sun exposure died following a melanoma diagnosis, compared to only 10% of those with high exposure habits. This represents an eight-fold increased risk of all-cause mortality for the “avoiders,” suggesting that the sun is not the driver of melanoma lethality, but rather a protective metabolic signal.
This is an observational study, and the author correctly identifies that it is difficult to separate an active sun-exposure habit from a generally active, healthy lifestyle. However, the dose-dependency observed across 29,518 women over two decades—showing protection against cardiovascular disease, type-2 diabetes, and venous thromboembolism—suggests a physiological mechanism beyond mere lifestyle confounding. Whether through vitamin D synthesis or other photo-metabolic pathways, the 1- to 2-year increase in life expectancy for sun-seekers is a signal that cannot be ignored.
I am a strong advocate for the safety of sun exposure if done carefully – start early at low UV, and build up a tan. No different than I advocate for exercise in someone who is deconditioned.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This narrative review summarizes over 20 years of research from the Melanoma in Southern Sweden (MISS) cohort, suggesting a strong, dose-dependent inverse relationship between sun exposure and all-cause mortality. The data indicates that women with active sun exposure habits have a 1- to 2-year longer life expectancy , primarily due to a lower risk of death from cardiovascular disease (CVD) and non-cancer causes. Most provocatively, the authors suggest that avoiding sun exposure is a risk factor for death of a similar magnitude to smoking. While these findings challenge current clinical guidelines that emphasize UV avoidance, they are observational and cannot definitively prove that sun exposure causes increased longevity, as “healthy lifestyle” bias remains a potential confounder.
Key Themes & Evidence Summary
- Scope: The review covers the evolution of the MISS study, investigating the impact of UV exposure on venous thromboembolism (VTE), type-2 diabetes (T2DM), endometrial cancer, and major causes of death (CVD, cancer, and non-CVD/non-cancer).
- Cardiovascular and All-Cause Mortality: Avoidance of sun exposure was associated with a 2-fold increase in mortality rate compared to the highest exposure group. This was driven by a 60% increased risk of CVD death and a significant increase in non-CVD/non-cancer death for sun avoiders.
- The “Smoking” Comparison: Life expectancy analysis showed that non-smokers who avoided the sun had a similar life expectancy to smokers with the highest sun exposure.
- Skin Cancer Paradox: While UV exposure increases melanoma incidence, low sun exposure and low vitamin D levels are linked to more aggressive melanomas and an eight-fold increased risk of all-cause mortality following a melanoma diagnosis.
- Pregnancy and Perinatal Health: The review highlights associations between vitamin D deficiency (often resulting from low sun exposure) and increased risks of eclampsia, pre-eclampsia, and newborn asphyxia.
Assertive Critical Appraisal
- Evidence Level: This is a Narrative Review (Level 5 Evidence), summarizing specific longitudinal cohort data and related literature.
- Quality Assessment (SANRA Scale):
- Justification & Aims: The review clearly justifies the need to re-evaluate sun exposure guidelines based on emerging mortality data.
- Literature Search: The search strategy is not explicitly described; the review focuses heavily on the author’s own MISS cohort publications. This introduces a significant risk of selection bias.
- Referencing: Key statements regarding hazard ratios, life expectancy, and physiological mechanisms (e.g., Vitamin D synthesis) are consistently supported by references.
- Scientific Reasoning: The argument is logically structured, moving from specific disease states to all-cause mortality. However, the author acknowledges the “major drawback” is the inability to fully separate a healthy lifestyle from sun exposure habits.
- Data Presentation: The review uses appropriate metrics, including Hazard Ratios (HR) and restricted mean survival time, and provides context for findings.
Research Objective
The aim of this review was to present the cumulative evidence leading to the conclusion that an inverse relationship exists between sun-exposure habits and all-cause mortality.
Bibliographic Data
- Title: The Winding Path Towards an Inverse Relationship Between Sun Exposure and All-cause Mortality
- Author: Pelle G. Lindqvist
- Journal: Anticancer Research
- Year: 2018
- DOI: 10.21873/anticanres.12337
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
