Comment:
I’ve always looked at the sun as a natural physiological signal rather than something we should instinctively fear. Our bodies evolved under it, and it makes clinical sense that gradual, low-dose exposure acts as an adaptive tonic for our health. I advocate going out in the early Spring, and building up a base tan, which I find becomes easier year to year as the skin remembers. The interesting tension in this Immunology paper is how a very real adaptive immune benefit gets complicated by the choice of subject (albino mice) and an artificial lab timeline.
The Adaptive Signal is Real
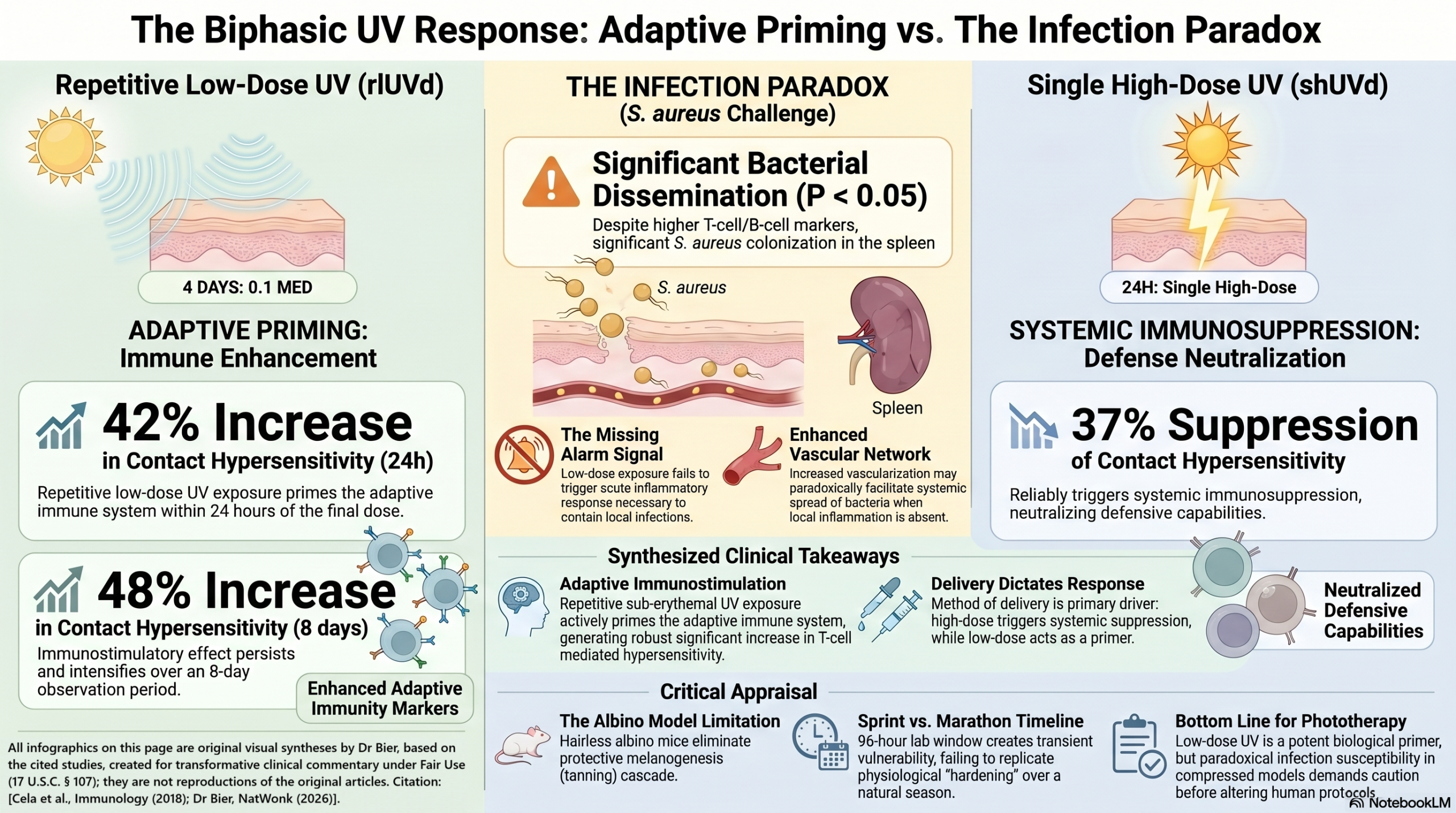
The study actually provides some great data supporting the idea of building a “base.” While a single high dose of UV (2.0 MED, like a bad sunburn) predictably shut down immune markers, a daily, low-dose protocol (0.1 MED for 4 days) did the exact opposite. It actually stimulated the adaptive immune response, bumping up contact hypersensitivity by 42% to 48% and enhancing specific antibody levels. It’s a elegant look at how low-intensity, frequent exposure primes our immune system rather than suppressing it. What has to be recognized is that the mice used are albino, so any protective impact of melanogenesis is absent.
The Problem with the 4-Day Window
Where the study gives me pause is the “Infection Paradox” they observed, where the low-dose mice had more bacterial dissemination to the spleen when challenged with S. aureus. The authors note that the low-dose exposure didn’t trigger the acute, inflammatory “alarm bells” that usually keep a local infection contained.
But this is where we have to look at the timeline with a healthy dose of clinical skepticism. A 4-day window in a lab just doesn’t match real life. In the real world, we build a base tan gradually over months of Spring and Summer, and across years of seasons. That kind of long-term, natural exposure allows for a structural hardening of the skin barrier and tanning, leading to a balanced immune equilibrium that a 96-hour albino mouse model simply can’t replicate. I understand that a short study is less expensive and allows researchers to churn out more publications, but it creates misleading results.
The Takeaway
Ultimately, the study confirms something valuable: low-dose sun exposure is a powerful primer for adaptive immunity. I am highly skeptical of the idea that gradual sun exposure puts a patient at a higher risk for systemic infections long-term. While a 4-day lab model shows a temporary vulnerability before the full immune infrastructure is built, a true season of natural exposure offers positive, protective clinical consequences. We just need to value the marathon of seasonal change over the sprint of a short lab protocol.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This animal model study demonstrates that the schedule and dosage of ultraviolet radiation (UVr) exposure fundamentally change the immune response. While a single high-dose exposure (shUVd) — simulating a sunburn — induces expected systemic immunosuppression, repetitive very low doses (rlUVd) — simulating short daily sun exposure — actually stimulate adaptive T-cell and B-cell responses. However, this “enhanced” adaptive immunity did not translate to better protection against Staphylococcus aureus; in fact, rlUVd-exposed mice showed increased bacterial dissemination to the spleen, likely because the lack of an initial inflammatory “warning” signal allowed the pathogen to bypass reinforced skin barriers and enter an enhanced vascular network.
Results in Context
- Main Results:
- rlUVd (0.1 MED x 4 days): Induced a 42% to 48% increase in contact hypersensitivity (CHS) and increased specific IgG3 antibody titers against tetanus toxoid.
- shUVd (2.0 MED x 1 day): Caused a 37% suppression of the CHS response and decreased specific total IgG and IgG2b levels.
- Definitions:
- Odds Ratio/Relative Risk Equivalent: In this study, “immunostimulation” or “suppression” percentages refer to the change in ear swelling (T-cell response) relative to sensitized, non-irradiated controls.
- MED (Minimal Erythemal Dose): The threshold dose of UVr required to produce visible skin reddening (damage).
- Participants: The study utilized male Crl:SKH1-hrBR hairless mice (n=5 per group for most experiments).
Assertive Critical Appraisal
- Limitations & Bias (STROBE Framework):
- Confounding: As a controlled laboratory experiment, environmental confounding was minimized; however, the use of hairless mice, while standard for dermatology, may not fully replicate the complex light-filtering properties of human skin or the presence of hair follicles which are active immune sites.
- Selection Bias: No explicit randomization method was described for assigning mice to the different irradiation protocols, which is a minor but notable reporting omission.
- Reporting Quality Assessment (STROBE):
- The authors clearly describe efforts to address confounding through standardized housing and irradiation spectrum controls (302 nm peak).
- Major Flaw/Omission: While the authors address confounding well, the sample size is relatively small (n=5-7 per group). This limits the power to detect subtle differences in cytokine profiles, particularly in the spleen where no significant differences were found despite changes in cell populations.
- Applicability:
- The findings regarding S. aureus are highly relevant to clinical concerns about skin infections. The observation that “reinforced” skin (thicker epithelium) can still be more susceptible to systemic dissemination due to increased vascularization and lack of early inflammation provides a cautionary note for phototherapy.
- The “immunostimulatory” effect of low-dose UV on vaccination (tetanus toxoid) is provocative but requires human validation before clinical implementation.
Research Objective
To evaluate and compare the effects of single high-dose vs. repetitive very low-dose UV radiation on systemic adaptive immunity (T-cell and B-cell responses) and the subsequent ability to control a cutaneous S. aureus infection.
Study Design
Observational and experimental animal study using three groups:
- shUVd: 400 $mJ/cm^2$ (2 MED) once.
- rlUVd: 20 $mJ/cm^2$ (0.1 MED) for 4 consecutive days.
- Control: Non-irradiated. Immune responses were assessed via flow cytometry, CHS reactions, ELISA for antibody titers, and a live-pathogen challenge model.
Setting and Participants
- Setting: Cátedra de Inmunología, Universidad de Buenos Aires, Argentina.
- Participants: 7-9 week old male Crl:SKH1-hrBR hairless mice.
- Dates: Study received August 2017, revised December 2017.
Bibliographic Data
- Title: Daily very low UV dose exposure enhances adaptive immunity, compared with a single high-dose exposure. Consequences for the control of a skin infection
- Authors: Eliana M. Cela, Cintia Daniela Gonzalez, Adrian Friedrich, Camila Ledo, Mariela Laura Paz, Juliana Leoni, Marisa Inés Gómez, and Daniel H. González Maglio
- Journal: Immunology
- Year: 2018
- DOI: 10.1111/imm.12901
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
