Comment:
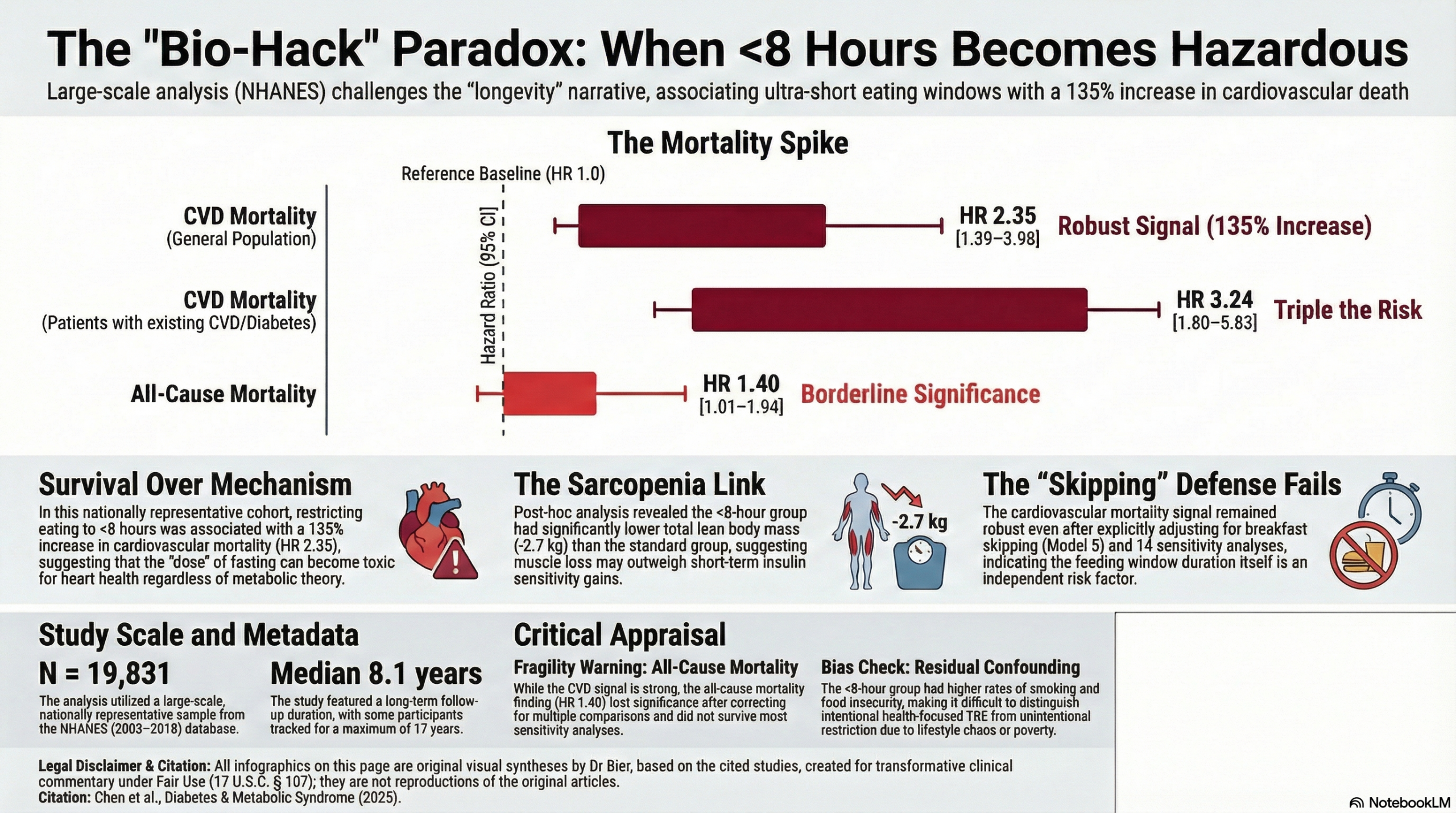
We are currently witnessing a significant conflict between the “biohacking” narrative—which promotes ultra-short eating windows (<8 hours) for longevity and metabolic optimization—and the hard clinical endpoints presented in this large-scale observational study. While the biochemical mechanisms of Time-Restricted Eating (TRE) are plausible in animal models, the hierarchy of evidence demands that we prioritize human survival data over mechanistic theory. The results here are stark: restricting food intake to less than 8 hours per day was associated with a massive 135% increase in the risk of cardiovascular mortality (HR 2.35 [95% CI, 1.39–3.98]) compared to a standard 12–14 hour window.
It Is Not Just “Skipping Breakfast”
A common reflex in nutritional epidemiology is to dismiss negative findings on fasting as a proxy for “disordered eating” or simply skipping breakfast. This study specifically stress-tested that assumption. The authors explicitly adjusted for breakfast skipping in their fully adjusted model (Model 5), and the strong association with cardiovascular death remained significant. Furthermore, the signal survived 14 distinct sensitivity analyses, including adjustments for meal frequency, snack frequency, and total energy intake. We cannot attribute this mortality risk to caloric deficit or the absence of a morning meal; the data identifies the short duration of the feeding window as a persistent risk factor even after controlling for these variables.
The Hierarchy of Harm: Overall Survival
While the authors highlight that the all-cause mortality signal was less robust than the cardiovascular signal in sensitivity analyses, the fully adjusted primary model still revealed a concerning trend: eating duration <8 hours was significantly associated with a 40% increased risk of all-cause mortality (HR 1.40 [95% CI, 1.01–1.94]). This directly challenges the primary claim of TRE proponents—that compressed eating windows extend lifespan. The data here suggests the opposite: a significant survival penalty.
Until randomized controlled trials can demonstrate safety on hard endpoints, strict <8-hour eating windows should be viewed with skepticism, particularly for those with existing cardiovascular risks.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This observational study identifies a concerning association between a daily eating duration of <8 hours and significantly increased risks of mortality. While a 91% increase in cardiovascular mortality was found to be robust across multiple sensitivity analyses, an observed 40% increase in all-cause mortality should be interpreted with significant caution. The all-cause mortality finding is considered “fragile” as it did not survive the majority of the authors’ sensitivity analyses and lost statistical significance after correcting for multiple comparisons. While time-restricted eating (TRE) is popular for short-term metabolic gains, these data suggest potential long-term risks, particularly regarding cardiovascular health and lean muscle preservation.
Results in Context
Main Results
The following hazard ratios (HR) compare participants eating <8 hours daily to those with a standard 12–14 hour window:
- Cardiovascular Mortality: HR 2.35 (95% CI, 1.39–3.98; P=0.002). This indicates a 135% increase in the risk of cardiovascular death.
- All-Cause Mortality: HR 1.40 (95% CI, 1.01–1.94; P=0.04). This suggests a 40% increase in the risk of death from any cause, though this finding was statistically marginal and less robust than the cardiovascular result.
- Cancer Mortality: HR 1.27 (95% CI, 0.66–2.47; P=0.47). No statistically significant association was observed.
- Lean Body Mass: In a post-hoc analysis, the <8-hour group had significantly lower total lean body mass (-2.7 kg) compared to the 12–14 hour group.
Definitions
- Hazard Ratio (HR): A relative measure of the rate at which events (deaths) occur in the treatment group versus the control group over time.
- Eating Duration: The time from the first to the last reported eating occasion (consuming >5 kcal) in a 24-hour period, averaged over two recall days.
Participants
- The study analyzed 19,831 adults from the NHANES (2003–2018).
- The median follow-up was 8.1 years, with a maximum of 17 years.
Assertive Critical Appraisal
Limitations & Bias (STROBE Framework)
- Measurement Bias: Diet was assessed via two 24-hour recalls. This may not capture long-term habitual patterns and is prone to recall error.
- Fragility of All-Cause Mortality: Unlike the cardiovascular result, the all-cause mortality association failed most sensitivity analyses and was non-significant (P=0.06) after applying the Benjamini-Hochberg correction for multiple testing.
- Residual Confounding: The <8-hour group had higher rates of smoking and food insecurity, and lower diet quality. While adjusted for, these factors (and the inability to distinguish intentional TRE from unintentional restricted eating) may still bias the results.
Reporting Quality Assessment (STROBE)
- Confounding Efforts: The authors used five sequential models to adjust for demographics, socioeconomic status, lifestyle, comorbidities, and even breakfast skipping.
- Sensitivity Analyses: The study included 14 sensitivity analyses, which is a high standard for testing the “sturdiness” of observational findings.
Applicability
- The sample is nationally representative of the US population, making it highly relevant to US general practice. However, results might not generalize to countries with significantly different dietary cultures.
Research Objective
To investigate the long-term association between daily eating duration (specifically <8 hours) and the risk of all-cause and cause-specific mortality.
Study Design
This was a prospective cohort study using data from the National Health and Nutrition Examination Survey (NHANES) linked to the National Death Index.
Setting and Participants
- Setting: Non-institutionalized civilian resident US population.
- Eligibility: Non-pregnant adults (≥20 years) with two valid dietary recalls representing usual intake.
- Exclusions: Individuals with extreme or implausible daily caloric intakes.
Bibliographic Data
- Title: Association of eating duration less than 8 h with all-cause, cardiovascular, and cancer mortality
- Authors: Meng Chen, Lan Xu, Linda Van Horn, JoAnn E. Manson, Katherine L. Tucker, Xihao Du, Nannan Feng, Shuang Rong, Victor W. Zhong
- Journal: Diabetes & Metabolic Syndrome: Clinical Research & Reviews
- Year: 2025 (Article in Press)
- DOI: https://doi.org/10.1016/j.dsx.2025.103278
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
