Comment:
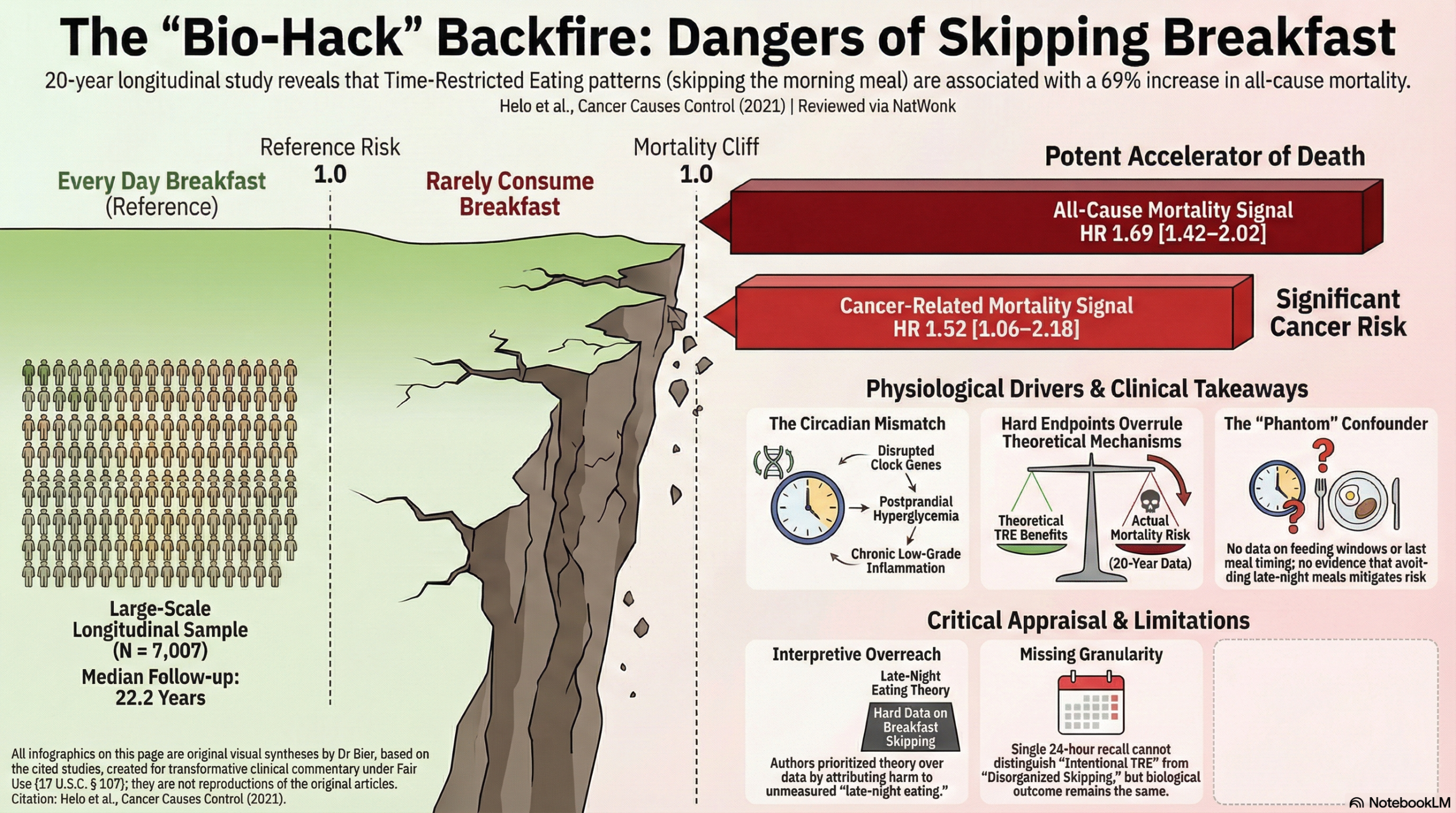
The current narrative surrounding Time-Restricted Eating (TRE) often relies on short-term metabolic markers or mechanistic theories to justify skipping the morning meal, but this massive prospective cohort study forces us to confront the hierarchy of clinical evidence: hard mortality endpoints consistently trump biochemical plausibility. In a nationally representative sample of over 7,000 adults followed for more than two decades, skipping breakfast wasn’t a “bio-hack” for longevity; it was a potent accelerator of death. The data revealed a 69% increase in all-cause mortality and a 52% increase in cancer-related mortality for those who rarely consumed breakfast compared to daily consumers.
What makes this paper particularly frustrating is the authors’ attempt to soften their own findings in the discussion which we’ve seen in other articles. Despite their data clearly associating the omission of breakfast with significantly reduced survival, they pivot to a rationalization that the harm is likely driven by “late-night dinners” or “circadian disruption” rather than the fasting itself. This is a critical overreach as the study methodology did not capture feeding windows, the timing of the last meal, or the intentionality behind the skipping. By suggesting that “intentional” fasting might still be safe based on external, short-term chemotherapy trials, they are prioritizing theoretical mechanisms over the hard epidemiological signal they just uncovered.
We need to look at the actual outcomes: in this cohort, the absence of a morning meal—regardless of the proposed mechanism—was not neutral or beneficial; it was deadly. We cannot ignore a hazard ratio of 1.69 based on the speculative hope that “doing it properly” yields a different result when the long-term human data suggests otherwise.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This prospective cohort study identifies a significant association between skipping breakfast and increased risks of all-cause mortality (69% increase) and cancer-related mortality (52% increase) among U.S. adults. While breakfast skipping is a common component of modern Time-Restricted Eating (TRE) or intermittent fasting regimens, this study suggests that “skipping” as a lifestyle habit—particularly when paired with late-night eating and poor diet quality—may have deleterious metabolic and oncogenic effects. Clinicians should note that while observational data cannot prove causation, the results highlight potential harms related to circadian rhythm disruption and impaired glucose metabolism associated with omitting the morning meal.
Results in Context
Main Results
The study followed 7,007 participants for a median of 22.2 years. After adjusting for age, sex, race, smoking, physical activity, BMI, and diet quality, the following risks were observed for those who rarely consumed breakfast compared to daily consumers:
- All-Cause Mortality: Hazard Ratio (HR) of 1.69 (95% CI: 1.42–2.02).
- Cancer-Related Mortality: HR of 1.52 (95% CI: 1.06–2.18).
Definitions: A Hazard Ratio (HR) of 1.69 indicates that at any given time, individuals who rarely ate breakfast were 69% more likely to die from any cause compared to those who ate breakfast every day, after accounting for other measured variables.
Harms Related to Breakfast Skipping (and by extension, TRE)
The authors posit several mechanisms by which skipping breakfast—a core tenet of many TRE protocols—might be harmful:
- Metabolic Disruption: Skipping breakfast is associated with postprandial hyperglycemia, elevated free fatty acids, and impaired insulin response after subsequent meals.
- Circadian Misalignment: Omitting the morning meal can disrupt the expression of “clock genes” that regulate hormone secretion and energy balance.
- Inflammatory Response: Prolonged fasting until midday may induce a state of physiological stress, leading to a low-grade inflammatory response.
- The “Late-Night” Confounder: Unlike structured TRE which often involves early-evening fasting, habitual breakfast skippers in the U.S. often consume late-night dinners. This pattern is linked to suppressed melatonin levels, which may promote tumor growth by reducing antioxidation and immunity.
Participants
- Total Sample: 7,007 adults aged ≥40 years.
- Baseline Habits: 16% rarely ate breakfast, 23% some days, and 61% every day.
Assertive Critical Appraisal
Limitations & Bias (STROBE Framework)
- Potential for Reverse Causality: Although the authors excluded those who died within 12 months of the baseline, it remains possible that individuals in poor health were more likely to skip breakfast.
- Confounding by Lifestyle: Breakfast skippers were more likely to be current smokers, obese, physically inactive, and have lower diet quality. While researchers adjusted for these factors, residual confounding is highly likely; skipping breakfast may simply be a proxy for a less health-conscious lifestyle.
- Self-Reported Exposure: Dietary data relied on a single 24-hour recall. This may not accurately reflect long-term habitual behavior and introduces potential misclassification bias.
Reporting Quality Assessment (STROBE)
The study generally adheres to STROBE principles. However, the authors did not adequately describe efforts to address unmeasured confounding beyond the calculation of E-values. The E-value for cancer mortality (2.56) suggests that an unmeasured confounder would need a moderately strong association with both the exposure and outcome to nullify the results.
Applicability
The findings are based on a nationally representative U.S. cohort (NHANES III), making the associations highly relevant to general clinical practice in the United States. However, clinicians must distinguish between the habitual skipping observed here and intentional TRE, which often involves higher diet quality and specific fasting windows.
Research Objective
To examine the association of breakfast skipping frequency with all-cause and cancer-specific mortality in U.S. adults.
Study Design
Prospective Cohort Study utilizing data from the Third National Health and Nutrition Examination Survey (NHANES III, 1988–1994) with mortality follow-up through 2015.
Setting and Participants
- Setting: Non-institutionalized U.S. population.
- Eligibility: Adults ≥40 years with no history of cancer or cardiovascular disease at baseline.
Bibliographic Data
- Title: The association of skipping breakfast with cancer-related and all-cause mortality in a national cohort of United States adults
- Authors: Dena Helo, Linda Appiah, Kishor M. Bhende, Theresa L. Byrd, Duke Appiah
- Journal: Cancer Causes & Control
- Year: 2021
- DOI: https://doi.org/10.1007/s10552-021-01401-9
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
