Comment:
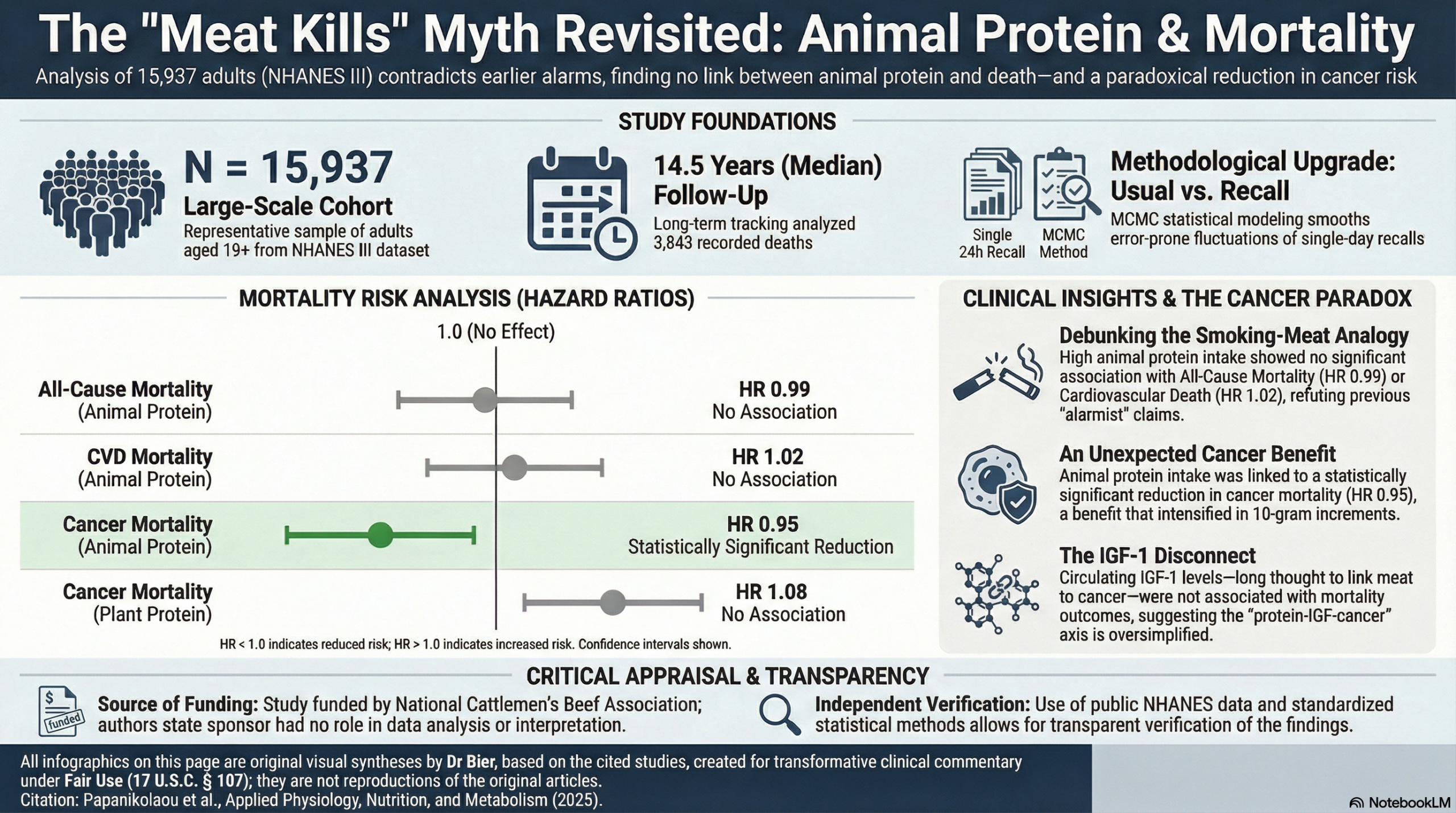
Another study showing that animal protein intake does not increase death rates. In fact, this study links higher animal protein intake to a reduced risk of cancer, albeit small. This study was designed specifically to revisit the controversial 2014 Levine findings that suggested a four-fold cancer risk from animal protein. By applying more sophisticated statistical procedures to the same NHANES III dataset, the researchers found that those alarming risks were likely artifacts of uneven group sizes and a failure to account for day-to-day dietary variation. The “meat is dangerous” signal vanishes when the data is cleaned of measurement error.
The results are a total reversal of previous claims. Not only was animal protein innocent of increasing all-cause or CVD mortality, it demonstrated a mildly protective effect against cancer (HR 0.95). Furthermore, the study confirmed that mortality risk was not associated with circulating IGF-1 in any age group, directly contradicting the theory that protein-driven IGF-1 is a mortality driver. These findings remained unchanged when separating the cohort into younger and older groups.
The clinical reality is that the fear of animal protein was built on a foundation of statistical noise. The definitive takeaway is that both animal and plant proteins are safe and appropriate for the general adult population.
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
