Comment:
This genotype study once again contradicts the prevailing narrative that meat is a universal cognitive toxin, and even it’s negative impact on all-cause mortality.
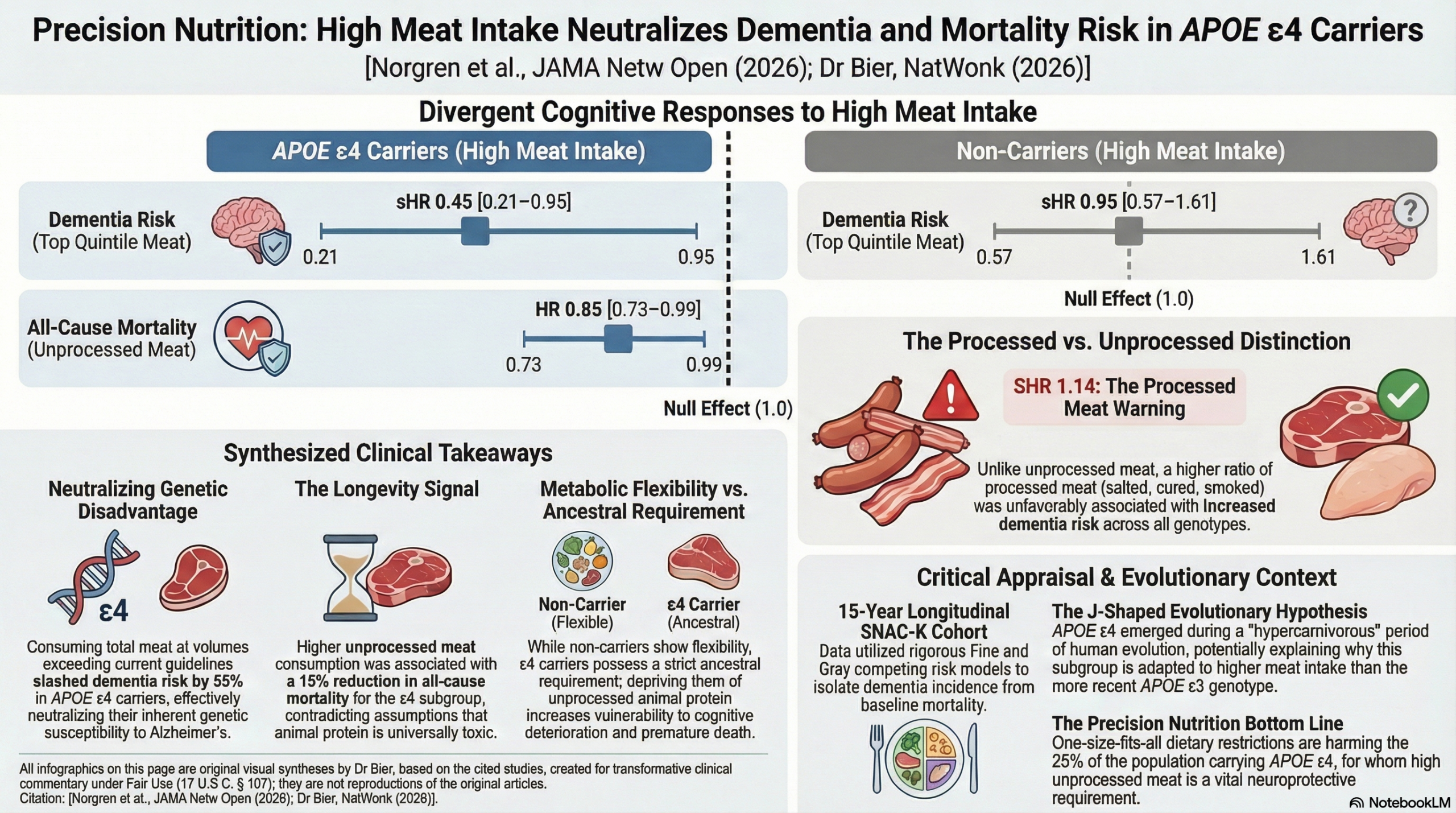
The findings from this 15-year Swedish cohort are unequivocal. There is absolutely no genetic subgroup in this study where higher total meat consumption increased the risk of dementia. In fact, for APOE ε4 carriers, the top quintile of meat intake effectively neutralized the genetic disadvantage typically seen in Alzheimer’s risk.
While a higher ratio of processed meat remained unfavorably associated with dementia across all genotypes (SHR = 1.14), unprocessed red meat and poultry demonstrated a protective signal. Processed and unprocessed meats are nutritional different foods.
Analytical and Physiological Filters
Applying a physiological filter, we see that the metabolic flexibility of non-carriers allows for null outcomes, but the ancestral requirements of carriers appear to demand high-quality animal protein. We must apply an analytical filter to the following outcomes observed in high-risk APOE ε4 carriers:
-
Mortality Reduction: Higher unprocessed meat consumption was associated with a 15% reduction in all-cause mortality (HR = 0.85), and was not associated with an increased mortality in any other group. There was even a non-significant trend towards improvement.
-
Cognitive Preservation: The intervention significantly slowed cognitive decline (beta = 0.32).
-
Safety Profile: Meat consumption did not increase dementia risk in any group, including non-carriers.
A dietary pattern that significantly lowers the risk of death while simultaneously preserving global cognition cannot be dismissed as “unhealthy.”
Mirroring and the “Healthy User” Mirage
Mirroring the Healthy User Bias against these results shows that even when accounting for overall diet quality (using metrics like the Alternative Healthy Eating Index), the meat-specific benefit for carriers remains robust. This suggests the benefit is not merely a statistical artifact of “healthier” people eating more meat, but a direct physiological interaction.
The definitive takeaway is that unprocessed meat is a net positive. For millions of patients with specific genetic profiles, “guideline-exceeding” levels of consumption are not a vice—they are a requirement for long-term neuroprotection.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line
This longitudinal cohort study suggests a significant gene-diet interaction between meat consumption and cognitive health. For the approximately 25% of the population carrying the APOE ε3/ε4 or ε4/ε4 genotypes, higher total meat consumption—exceeding current dietary guidelines—was associated with slower cognitive decline and a 55% reduction in dementia risk. Conversely, no such benefit was observed in individuals with other APOE genotypes. Clinicians should note that while unprocessed meat appeared protective for this high-risk genetic subgroup, a higher ratio of processed meat remained unfavorably associated with dementia risk across all genotypes. These findings support the emerging field of precision nutrition, suggesting that “one-size-fits-all” dietary meat restrictions may inadvertently disadvantage individuals with specific ancestral genetic profiles.
Results in Context
- Main Results (APOE34/44): Among participants with APOE ε3/ε4 or ε4/ε4 genotypes, the highest quintile of meat consumption (Q5) compared to the lowest (Q1) was associated with:
- Better cognitive trajectories: ß = 0.32 (95% CI, 0.07 to 0.56; P = .01).
- Reduced dementia risk: Subdistribution Hazard Ratio (SHR) of 0.45 (95% CI, 0.21 to 0.95; P = .04).
- Main Results (Non-carriers): No significant associations were found for individuals with APOE ε2/ε2, ε2/ε3, ε2/ε4, or ε3/ε3 genotypes (Cognition: P = .20; Dementia: P = .86).
- Processed vs. Unprocessed Meat: A higher ratio of processed to total meat was associated with an increased risk of dementia (SHR 1.14; 95% CI, 1.01 to 1.29; P = .04), with no significant APOE interaction observed for this specific metric.
- Mortality: Post hoc analyses found that higher unprocessed meat consumption was associated with reduced all-cause mortality exclusively in the APOE34/44 group (HR 0.85; 95% CI, 0.73 to 0.99; P = .04).
Definitions
- beta (Regression Coefficient): In this study, this represents the estimated difference in the rate of cognitive change (z-score) per 10 years between groups. A positive ß indicates a more favorable (slower) decline.
- SHR (Subdistribution Hazard Ratio): Used in “Fine and Gray” models to estimate the risk of an event (dementia) while accounting for the “competing risk” of death (dying before a dementia diagnosis can occur).
- Quintiles (Q1–Q5): The study divided meat intake into five equal groups. Q1 represents the lowest intake, and Q5 represents the highest.
Assertive Critical Appraisal
Limitations & Bias (STROBE Framework)
- Confounding: The authors adjusted for a wide array of covariates, including age, sex, education, physical activity, and overall diet quality (AHEI score). However, as an observational study, residual confounding from unmeasured lifestyle or socioeconomic factors cannot be entirely excluded.
- Self-Reported Diet: Dietary data were collected via food-frequency questionnaires, which are prone to recall bias. However, the authors argue this is unlikely to vary by APOE status, meaning it would likely blunt rather than create the observed interaction.
- Reverse Causality: There is a risk that individuals in the early, undiagnosed stages of dementia might change their diet. The authors attempted to mitigate this by using a 15-year follow-up and conducting sensitivity analyses excluding early cases, which yielded consistent results.
Reporting Quality Assessment (STROBE)
- Strengths: The study performed exceptionally well in describing efforts to address confounding, utilizing a “triangulation approach” that compared between-participant and within-participant (crossover-style) analyses.
- Methodological Detail: The use of “Fine and Gray” models to account for the competing risk of death is a robust choice for geriatric populations where mortality is high.
Applicability
- The study population was predominantly Northern European (Stockholm, Sweden), which may limit generalizability to other ethnic groups with different ancestral dietary patterns or APOE-related risk profiles.
- The findings are particularly relevant given that the high-meat consumption levels (Q3–Q5) that showed benefit in carriers actually exceed current national guidelines.
Research Objective
To test the hypothesis that higher meat consumption is associated with better cognitive health specifically in individuals with APOE ε3/ε4 and ε4/ε4 genotypes, and to compare this association with other APOE genotypes.
Study Design
A population-based cohort study using 15 years of longitudinal data from the Swedish National Study on Aging and Care-Kungsholmen (SNAC-K). The study used repeated exposure measures (diet) and outcomes (cognition/dementia).
Setting and Participants
- Location: An urban area of Stockholm, Sweden.
- Participants: 2157 adults aged 60+ without dementia at baseline.
- Follow-up: Participants were assessed every 3 to 6 years over a 15-year period.
Bibliographic Data
- Title: Meat Consumption and Cognitive Health by APOE Genotype
- Authors: Jakob Norgren, Adrián Carballo-Casla, Giulia Grande, Anne Börjesson-Hanson, Hong Xu, Maria Eriksdotter, Erika J. Laukka, Sara Garcia-Ptacek
- Journal: JAMA Network Open
- Year: 2026
- DOI: 10.1001/jamanetworkopen.2026.6489
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
