Comment:
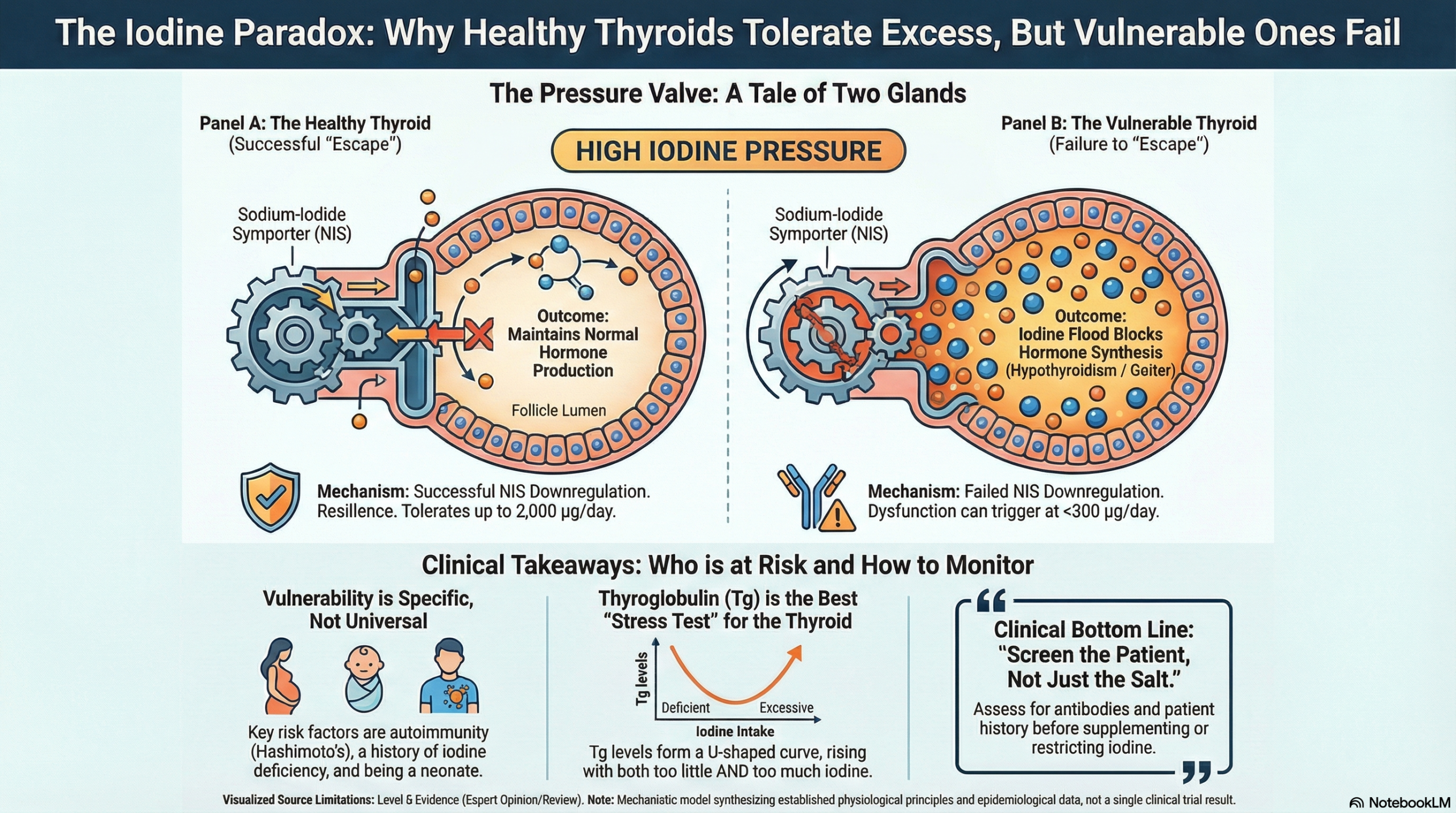
It is ‘common knowledge’ that higher iodine supplementation is dangerous. However this review clearly shows the distinction between the ‘healthy majority’ and the ‘vulnerable minority.’ While most individuals possess a robust capacity to handle high iodine loads (via the Wolff-Chaikoff escape mechanism), the data here is a reminder that doesn’t apply for specific subgroups. For patients with underlying autoimmunity or a history of deficiency, that adaptation fails—converting a nutrient surplus into a trigger for hypothyroidism and Hashimoto’s. It suggests our clinical focus shouldn’t be on restricting iodine universally, but on rigorously screening for that vulnerability before supplementing.
The Wonk Debate – Audio Critique & Clinical Commentary:
Summary:
Clinical Bottom Line:
This narrative review argues that while universal salt iodization has remarkably improved global health, the relationship between iodine intake and thyroid pathology follows a U-shaped curve. The authors conclude that while most healthy euthyroid individuals can tolerate high iodine intakes (up to 2 g/day) well due to effective autoregulation, specific subgroups—particularly those with pre-existing thyroid disease, a history of iodine deficiency, and neonates—are susceptible to thyroid dysfunction at intakes only slightly above physiological needs. The review emphasizes that while urinary iodine concentration (UIC) remains the standard for population monitoring, thyroglobulin (Tg) is a sensitive, U-shaped biomarker valuable for detecting thyroid stress from both deficiency and excess.
Key Themes & Evidence Summary
Scope:
The review outlines potential sources of excess iodine, including over-iodized salt, drinking water, animal milk, seaweed, and supplements. It details the physiological responses to excess iodine, specifically the Wolff-Chaikoff effect, and the consequences such as hyperthyroidism, hypothyroidism, and autoimmunity. It also evaluates biomarkers for assessment, focusing on UIC and Tg.
Key Arguments:
- Vulnerability: The risk of iodine-induced thyroid dysfunction is heavily modulated by prior iodine status. Populations introducing iodized salt into previously deficient areas are at a transiently increased risk for iodine-induced hyperthyroidism, which can occur at intakes less than 300 µg/day.
- Sources: Excess exposure is often unintended and cumulative. Groundwater iodine concentrations can vary significantly, sometimes being the principal source of dietary iodine. Milk products can be iodine-rich due to iodinated cattle fodder and iodophor disinfectants.
- Biomarkers: The median UIC is the recommended biomarker for identifying populations with excessive intakes. Thyroglobulin (Tg) follows a U-shaped association with iodine intake, rising in conditions of both deficiency and excess, making it a sensitive indicator of thyroid stress.
- Mechanism: In healthy thyroids, the Wolff-Chaikoff effect (acute inhibition of hormone synthesis) is transient, followed by an “escape” phenomenon. Failure to escape, often in those with underlying autoimmunity or prior deficiency, leads to hypothyroidism or goiter.
Increased Susceptibility to Dysfunction
- Individuals with pre-existing thyroid disease, including autoimmune thyroiditis, are considered a vulnerable group.
- They may be susceptible to thyroid disorders at iodine intakes that are only slightly above physiological needs, whereas healthy individuals can typically tolerate much higher levels.
Risk of Hypothyroidism
- Failure to Adapt: In people with underlying autoimmune thyroiditis (AT), acute excess iodine intake can lead to temporary overt or subclinical hypothyroidism. This occurs because vulnerable individuals may fail to “escape” from the acute Wolff-Chaikoff effect (the normal temporary inhibition of thyroid hormone synthesis in response to high iodine).
- Mechanism: In autoimmune thyroiditis, lymphocytic infiltration and stimulation by antithyroid antibodies can increase the risk of chronic inflammation and subsequent hypothyroidism when exposed to excess iodine.
Development or Exacerbation of Autoimmunity
- Risk Factor: Excessive iodine consumption is widely described as a risk factor for the development of thyroid autoimmunity.
- Population Studies: Studies have shown that following the introduction of iodized salt, there can be an increased incidence of thyroid antibody positivity and Hashimoto’s thyroiditis, particularly in populations previously exposed to iodine deficiency.
- Genetic Predisposition: The risk of developing autoimmunity from iodine exposure is higher in those with a genetic predisposition, and is more common in females.
Pregnancy and Postpartum Risks
- Postpartum Thyroiditis: Women with positive thyroid antibodies (TPOAb or TgAb) in the first trimester are at a sharply elevated risk (50% compared to 5% in healthy populations) of developing postpartum thyroiditis.
Assertive Critical Appraisal
- Evidence Level: This is a Narrative Review (Level 5 Evidence/Expert Opinion). While comprehensive, it represents the authors’ synthesis of the literature rather than a systematic meta-analysis of all available data.
- Quality Assessment (SANRA Scale):
- Justification & Aims: High. The importance is well-justified by the contrast between global iodization strategies and the risks of excess intake. The aims—to review etiology, responses, and biomarkers—are clearly formulated.
- Literature Search: High. Unlike many narrative reviews, the authors explicitly describe their search strategy, listing databases (PubMed, Web of Science, Scopus, etc.) and specific search terms (e.g., “iodine excess”, “thyroglobulin”), which enhances transparency.
- Referencing: High. Key statements regarding physiological mechanisms, epidemiological data, and clinical outcomes are supported by extensive referencing, with over 190 citations.
- Scientific Reasoning: High. The argument is logical, carefully distinguishing between effects in healthy adults versus susceptible groups like neonates and those with autoimmune susceptibility.
- Data Presentation: High. Data are presented effectively in tables, such as the recommended upper intake levels and biomarker thresholds, aiding clinical interpretation.
Research Objective:
The objective is to review the association between excess iodine intake and thyroid function, including etiology, physiological responses, and consequences, and to provide guidance on biomarkers for population monitoring, with an emphasis on UIC and Tg.
Bibliographic Data:
- Title: Excess iodine intake: sources, assessment, and effects on thyroid function
- Authors: Jessica Farebrother, Michael B. Zimmermann, and Maria Andersson
- Journal: Annals of the New York Academy of Sciences
- Year: 2019
- DOI: 10.1111/nyas.14041
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
