The Wonk Debate – Audio Critique & Clinical Commentary:
The “Metabolic Panacea” Delusion: When Fasting Signals Catabolism and Mortality
Updated: 1-25-2026
The “Metabolic Panacea” Delusion: When Fasting Signals Catabolism and Mortality
The current fervor surrounding Time-Restricted Eating (TRE) and Intermittent Fasting has created a profound Core Tension: a collision between the biochemical promise of “metabolic hacking” and the sobering reality of epidemiological survival data. While mechanistic theories suggest benefits like autophagy and improved insulin sensitivity, large-scale human models reveal a persistent mortality signal that cannot be ignored. Physiology is rarely linear; instead, it often follows a U-shaped curve where extremes in fasting duration transition from theoretical optimization to tangible physiological stress.
The Hierarchy of Harm: Prioritizing Survival Over Surrogate Markers
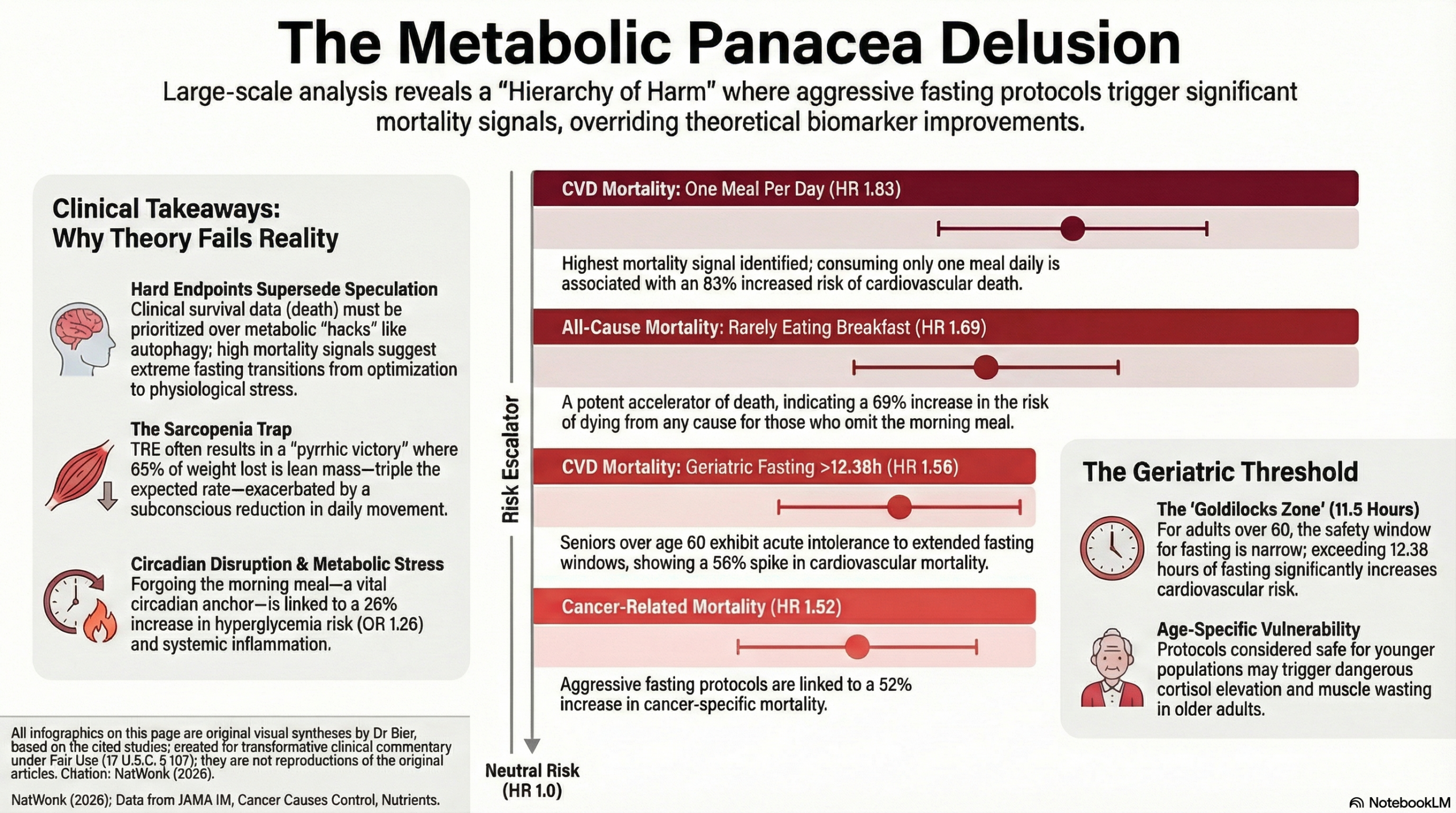
In biomedical research, hard clinical endpoints must always supersede mechanistic speculation. Recent data involving over 7,000 adults followed for over two decades highlights that skipping breakfast is a potent accelerator of death. Large-scale meta-analyses and prospective studies have identified distinct, escalating risk profiles:
-
All-Cause Mortality: Habitual breakfast skipping is associated with a 27% increase in all-cause mortality in some cohorts, while more recent longitudinal data shows a staggering 69% increase in all-cause mortality (HR 1.69) for those who rarely eat breakfast.
-
Cardiovascular Disease (CVD) Mortality: The risk is particularly acute for heart health, with studies showing a 49% increase in CVD mortality for breakfast skippers and an 83% increase for those consuming only one meal per day (HR 1.83).
-
Cancer Mortality: Aggressive fasting protocols and morning meal omission are linked to a 34% to 52% increase in cancer-specific mortality (HR 1.52).
Theoretical gains in biomarkers like weight loss or glucose do not override a mortality signal this strong in actual humans. Any protocol influencing human survival must be treated with the same skepticism as a new pharmaceutical; it is guilty of harm until proven innocent through high-quality survival data.
The “Sarcopenia Trap” and Behavioral Downregulation
Beyond survival, the composition of weight loss during TRE presents a critical safety signal. In randomized trials, approximately 65% of the weight lost during a 16:8 protocol was lean mass—far exceeding the 20–30% ratio typical of standard caloric restriction. This suggests that without specific protein pacing or resistance training, fasting may inadvertently accelerate sarcopenia.
This muscle loss is compounded by a behavioral “double hit”: patients in TRE groups often show a significant reduction in daily step counts, suggesting the body subconsciously downregulates non-exercise activity thermogenesis (NEAT) to conserve energy. Clinicians must recognize that weight loss achieved at the expense of metabolically active tissue and physical activity is a pyrrhic victory.
Circadian Disruption: The Price of Missing the Morning Meal
The proposed mechanism for these harms often centers on circadian misalignment. While proponents argue that “intentional” fasting differs from “unstructured” skipping, the body’s internal clock rarely makes this distinction. Forgoing the morning meal can lead to:
-
Metabolic Disruption: Skipping breakfast is associated with postprandial hyperglycemia, impaired insulin response, and a 26% increase in hyperglycemia risk (OR 1.26).
-
Systemic Hypertension: Skipping breakfast is linked to a 21% higher risk of hypertension (OR 1.21).
-
Inflammatory and Oncogenic Stress: Prolonged fasting until midday may induce physiological stress and low-grade inflammation. Furthermore, habits paired with breakfast skipping—like late-night eating—can suppress melatonin levels, potentially promoting tumor growth.
Missing the morning meal forces the body into a state of physiological pressure that appears to override the theoretical benefits of a longer fasting window. Until proven otherwise, the removal of the morning meal must be treated as a metabolic and oncogenic stressor.
Age-Specific Risks: The Geriatric “Goldilocks Zone”
The risks of aggressive fasting are particularly acute for the elderly. In adults over 60, fasting beyond just 12.38 hours is associated with a 56% increase in CVD mortality (HR 1.56). This population faces a “Goldilocks zone” for metabolic health—found at approximately 11.5 hours of overnight fasting. Extending this window likely triggers muscle catabolism and cortisol elevation, making standard 16:8 protocols uniquely hazardous for aging bodies.
The Verdict
The collective evidence suggests that aggressive Time-Restricted Eating, particularly when it involves skipping the morning meal, carries a significant and under-reported mortality risk. While short-term weight loss is possible, it is often achieved through the disproportionate loss of lean mass and at the cost of cardiovascular and oncogenic stability.
We cannot ignore a 69% increase in all-cause mortality based on the speculative hope that “intentional” fasting yields a different result. Clinicians should prioritize structured meal timing that respects circadian biology—starting with a consistent morning meal—over aggressive fasting regimens that chase surrogate markers while potentially compromising survival.
References
-
Helo, D., Appiah, L., Bhende, K. M., Byrd, T. L., & Appiah, D. (2021). The association of skipping breakfast with cancer-related and all-cause mortality in a national cohort of United States adults. Cancer Causes & Control, 32(12), 1435–1443. https://doi.org/10.1007/s10552-021-01401-9
-
Lowe, D. A., Wu, N., Rohdin-Bibby, L., Moore, S. S., Kelly, N., Liu, B. E., Philip, E., Vittinghoff, E., Heymsfield, S. B., Olgin, J. E., Kurpert, C. W., & Weiss, E. J. (2020). Effects of time-restricted eating on weight loss and other metabolic parameters in women and men with overweight and obesity: The TREAT randomized clinical trial. JAMA Internal Medicine, 180(11), 1491–1499. https://doi.org/10.1001/jamainternmed.2020.4153
-
Sun, Y., Rong, S., Liu, B., Du, Y., Wu, Y., Chen, L., Xiao, Q., Snetselaar, L., Wallace, R., & Bao, W. (2023). Meal skipping and shorter meal intervals are associated with increased risk of all-cause and cardiovascular disease mortality among US adults. Journal of the Academy of Nutrition and Dietetics, 123(3), 417–426. https://doi.org/10.1016/j.jand.2022.08.119
-
Wang, Y., Li, F., Li, X., Wu, J., Chen, X., Qin, T., Liu, X., Liang, L., Ma, J., & Qin, P. (2024). Breakfast skipping and risk of all-cause, cardiovascular and cancer mortality among adults: a systematic review and meta-analysis of prospective cohort studies. Food & Function, 15(1), 114–125. https://doi.org/10.1039/d3fo05705d
-
Yang, B., Lian, L., Xing, K., Cen, Y., Zhao, Y., & Zhang, Y. (2025). Association of skipping breakfast with metabolic syndrome and its components: A systematic review and meta-analysis of observational studies. Nutrients, 17(19), 3155. https://doi.org/10.3390/nu17193155
-
Zhang, H., Zhang, S., Liu, Y., Wang, X., & Hu, J. (2025). The association between skipping breakfast and cardiovascular disease: a meta analysis. Frontiers in Cardiovascular Medicine, 12, 1565806. https://doi.org/10.3389/fcvm.2025.1565806
-
Zhang, Z., Zhao, H., Tao, Z., Jiang, M., & Pu, J. (2024). A national study exploring the association between fasting duration and mortality among the elderly. Nutrients, 16(13), 2018. https://doi.org/10.3390/nu16132018
Fair Use & Copyright: This post provides a transformative, thesis‑driven critical appraisal intended for educational and scholarly purposes. It is not a reproduction of, nor a market substitute for, the original research article.
Support the Version of Record: To support the copyright holders and verify the underlying data—including primary survival curves, risk estimates, and other core outcomes—readers are strongly encouraged to access the original Version of Record via the link or DOI provided above.
Medical Disclaimer: This content is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment.
